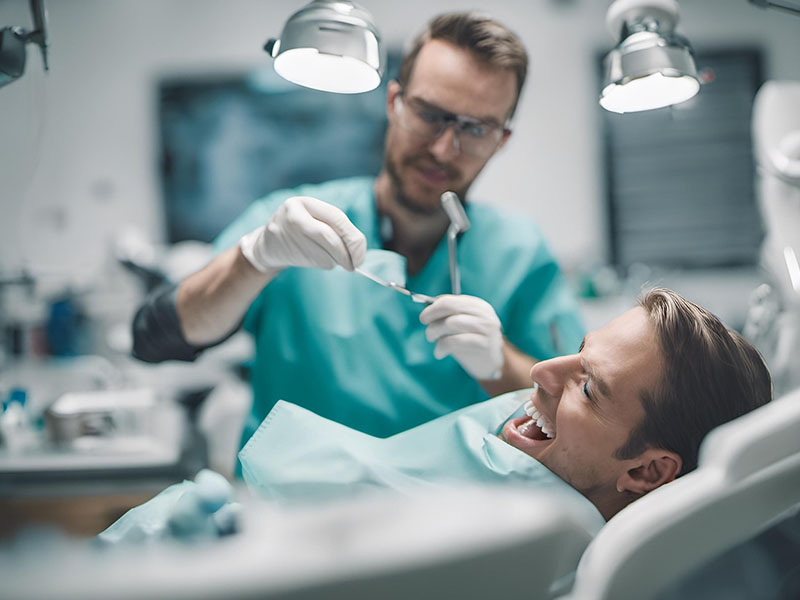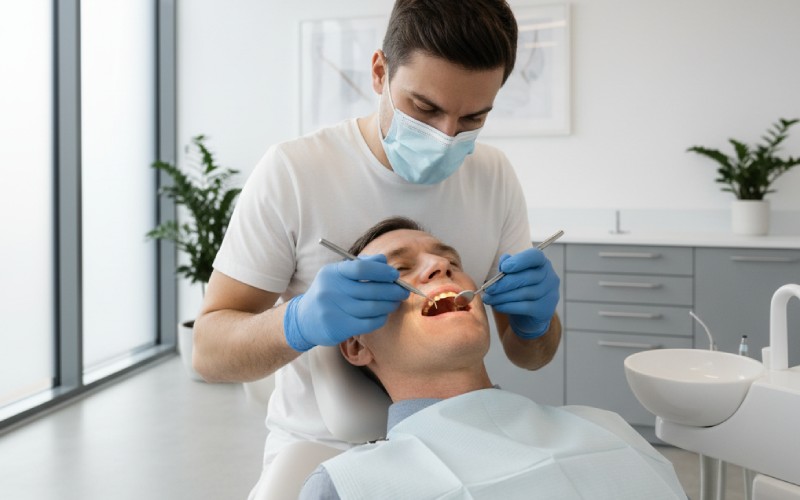
How Do Dentists Know If You Smoke? (Even If You Don’t Tell Them)
If you’ve ever sat in the dental chair wondering, “Can my dentist tell I smoke?” you’re not alone. A lot of people quietly worry about this – especially if they only smoke “socially” or they’re trying to cut down.
Here’s the blunt truth: Most dentists can usually tell if you smoke, even if you brush beforehand, pop a mint, and swear you’re “just an occasional smoker.” Smoking leaves a fingerprint in your mouth – in your teeth, gums, breath, and even how your mouth heals.
That said, your dentist is (or should be) a health partner, not a moral judge. They’re not trying to “catch you out” – they’re trying to protect you from very real problems like gum disease, tooth loss, and mouth cancer.
- In this guide, you’ll learn:
- 그리고 보이는 signs that instantly tell a dentist you smoke
- 그리고 subtle clues they see that you probably don’t
- How vaping, shisha and weed show up differently in your mouth
- Why your dentist actually asks about smoking (it’s not to lecture you)
- What you can do to protect your mouth – even if you’re not ready to quit yet
목차
Dentists Are Not Human Lie Detectors – They’re Pattern Readers
When a dentist looks in your mouth, they’re not just counting cavities. They’re reading patterns: colour, texture, smell, blood supply, how your gums attach to your teeth, how bone looks on X-rays, how wounds heal over time.
Smoking and other nicotine products change many of those patterns at once. Over the years, dentists see these changes in thousands of mouths, so they get very fast at thinking, “This looks like a smoker’s mouth.”
On top of that, we know from big public-health studies that people who smoke are much more likely to have gum disease, tooth loss and certain mouth lesions than non-smokers.
- The first things a dentist often notices if you smoke:
- Tooth staining that doesn’t brush off easily Tar and nicotine cling to enamel, causing yellow or brown stains, especially on front teeth and near the gumline.
- A very specific pattern of tartar (calculus) build-up Smokers tend to get heavier, darker deposits – especially behind lower front teeth and along the gumline.
- Gums that are inflamed but don’t bleed much Nicotine narrows blood vessels. That can “hide” bleeding even when gum disease is present, which is a classic smoker pattern.
- Persistent bad breath (halitosis) Smoke particles stick to soft tissues and mix with dry mouth and bacteria, creating a very recognisable odour.
- Brownish patches on the gums (smoker’s melanosis) This is a harmless but obvious brown/black pigmentation often seen on the lower front gums of tobacco users.
- White or thickened patches on the lining of the mouth Chronic irritation from smoke or smokeless tobacco can cause lesions such as leukoplakia or smoker’s keratosis, which dentists are trained to recognise.
The Subtle Signs – Even “Social Smokers” Leave Clues
You might think, “But I only smoke on nights out; surely they can’t tell?” The thing is, your mouth is very sensitive to toxins. For many people, even relatively low levels of exposure over time can leave traces.
Dentists see that smokers (even light or intermittent ones) are more likely to have early gum disease, reduced healing and characteristic staining patterns compared with non-smokers.
And because nicotine affects blood flow and immune function, your gums’ defence system simply doesn’t behave like a non-smoker’s – something that shows up clearly over years of check-ups and X-rays.
- “Invisible to you” clues dentists pick up on:
- Gum disease that looks calmer than it should Plaque and tartar levels say “this should be bleeding a lot,” but the tissues look strangely pale or fibrous – a smoker hallmark.
- Bone loss patterns on X-rays Smokers are more likely to have deeper bone loss around teeth, linked to severe periodontitis and future tooth loss.
- Slow or complicated healing after extractions or surgery Smoking increases the risk of problems like “dry socket” and infections after dental work.
- A history that doesn’t match your age Multiple missing teeth, frequent gum infections or repeated deep cleanings in someone who is otherwise healthy often point toward smoking or vaping.
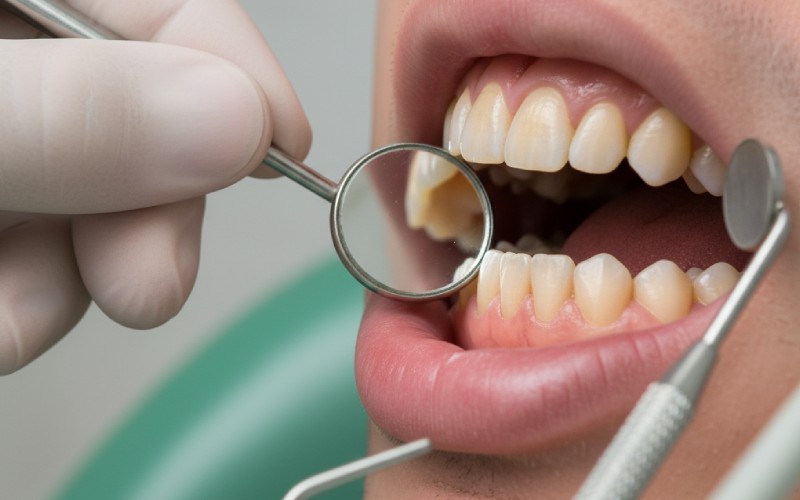
At-a-Glance: How Smoking Shows Up in Your Mouth
Here’s a quick overview of how dentists connect what they see with possible smoking habits:
| What your dentist sees | What it may suggest in a smoker | Can it improve if you quit?* |
|---|---|---|
| Yellow–brown tooth staining near gums | Tar/nicotine staining from cigarettes or other tobacco | Stains can be polished; new staining slows dramatically |
| Receding, “tough” gums | Long-term gum disease with reduced blood flow | Gums won’t “grow back,” but inflammation can improve |
| Heavy tartar along lower front teeth | drier mouth, more plaque and mineral deposits | New tartar forms more slowly with quitting and good care |
| Brown patches on gums (smoker’s melanosis) | Pigment changes triggered by tobacco use | Often fades within months–years of stopping |
| Frequent infections or dry socket after surgery | Impaired healing and immune response due to smoking | Healing response improves after quitting |
| Persistent bad breath despite brushing | Smoke in soft tissues + dry mouth + more gum disease bacteria | Breath usually improves within weeks of quitting |
*Improvement depends on your overall health, how long you’ve smoked and how advanced the damage is. Always follow your own dentist’s advice for your specific situation.
- Why dentists actually care whether you smoke (beyond “it’s bad for you”)
- Treatment planning: Smokers have higher risks of gum disease, tooth loss and oral cancer, so dentists tailor check-up frequency, X-rays and cleanings accordingly.
- Surgery and healing: Smoking affects blood flow and immune function, which can reduce the success of implants, gum surgery and extractions.
- Cancer screening: Because tobacco is a major risk factor for mouth cancer, dentists will be extra careful checking your tongue, cheeks, lips and throat area.
- Medication and anaesthetic decisions: They may adjust what they use or how they do a procedure if they know your healing could be slower.
- Helping you quit (if you want to): Many dental teams are trained to give brief advice, refer you to stop-smoking services or at least help you reduce harm.
“What About Vaping, Shisha, Weed, or Nicotine Pouches?”
A lot of people switch from cigarettes and assume, “Cool, my dentist won’t be able to tell anymore.” Not quite.
While vaping and other nicotine products may reduce some risks compared with traditional smoking, they still leave a trail in your mouth. Research and clinical experience show links between vaping, dry mouth, gum inflammation, plaque build-up and an increased risk of tooth decay, although the long-term effects are still being studied.
Cannabis (smoked) and shisha/hookah also expose your mouth to heat, tar and irritants, which can lead to gum disease, dry mouth and staining over time.
- How different habits can look in your mouth:
- Cigarettes / cigars: Classic yellow-brown staining, smoker’s melanosis, reduced gum bleeding despite disease, stronger “smoky” breath.
- Vaping (e-cigs): Less obvious staining, but more 구강 건조증, increased plaque, and sometimes inflamed gums or “vaper’s tongue” (altered taste).
- Smokeless tobacco (chew, snus): Localised gum recession and white or thickened patches exactly where the product sits.
- Cannabis smoking: Dry mouth, higher rates of gum disease, staining and, in some cases, characteristic inflammation patterns on the palate and gums.
Even if 당신 don’t notice much difference in the mirror, your dentist is looking with a very trained eye – plus they have your history, X-rays and years of patterns to compare.
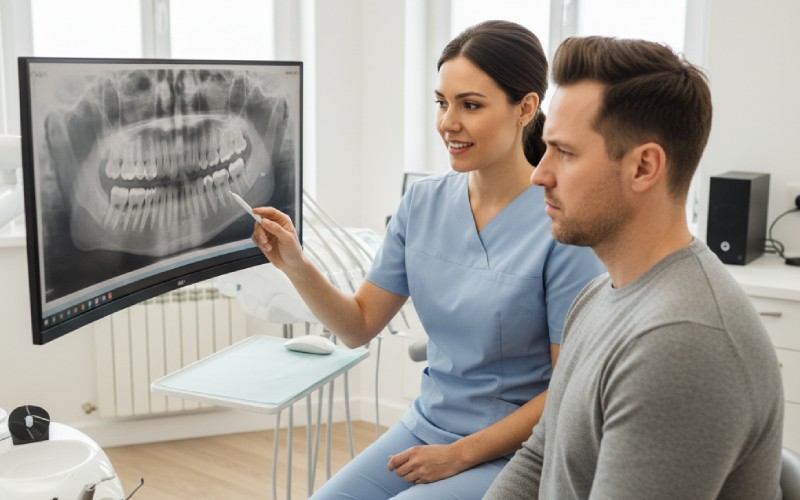
If You Smoke and You’re Nervous About the Dentist
Maybe you’re worried they’ll judge you. Maybe you’re scared they’ll “tell you off” or give you a big lecture. Maybe you’ve even skipped appointments because of it.
Here’s the thing: your dentist already sees the signs; what they really need is your honesty. Knowing how much 그리고 how often you smoke (or vape) helps them:
- catch problems earlier
- choose safer treatments
- give you realistic expectations about healing and long-term results
And if you’re trying to quit or cut down, that’s something most dentists genuinely want to support – not shame.
(This article is general information, not personal medical advice. For any decisions about your own health, always talk directly with your dentist, doctor or another qualified professional.)
- Not ready to quit? Here are realistic “next best” steps
- Keep your check-ups, even if you’re embarrassed Catching gum disease or precancerous changes early can literally save teeth – and sometimes lives.
- Upgrade your home care Brush twice daily with fluoride toothpaste, clean between teeth (floss or interdental brushes) and consider an alcohol-free mouthwash if your dentist recommends it.
- Time your smoking away from dental work Avoid smoking right before and for as long as possible after extractions, surgery or deep cleanings to support healing.
- Fight dry mouth Drink water regularly, chew sugar-free gum or lozenges to stimulate saliva, and ask your dentist about saliva substitutes if needed.
- Ask your dentist quietly about quitting options Even a short conversation can point you to nicotine-replacement therapy or stop-smoking services that actually fit your life.
Quick FAQs (The Things People Are Afraid to Ask)
“Can my dentist tell if I smoke only occasionally?” Often, yes – especially if “occasionally” has actually meant “on and off for years.” Even low levels of regular exposure can contribute to staining, gum changes and altered healing that dentists learn to recognise.
“Will my dentist judge me for smoking?” A good dentist won’t. Their job is to manage risk, protect your teeth and screen for serious disease – smoking is just one piece of that puzzle. If you ever do feel judged, it’s okay to seek a practitioner whose style feels more supportive.
“If I quit, will my mouth completely recover?” Some things can significantly improve or partially reverse – like inflammation, bad breath, and your risk of future tooth loss and mouth cancer. Other changes (like advanced bone loss or gum recession) are permanent, though they can be stabilised and treated.
결론
Dentists don’t need to be mind-readers to know you smoke. Your teeth, gums, breath, bone levels and healing response are quietly telling the story.
But this isn’t about catching you out. It’s about giving your mouth a chance – whether that means quitting now, cutting down, or simply doing the best you can today while you figure it out.
If you’re worried, the most powerful thing you can do at your next visit is simple and brave:
“I do smoke (or vape). I’m not ready to quit yet, but I want to keep my teeth as healthy as possible. What can we do?”
That one sentence turns your dentist from an imagined judge into what they were always meant to be: a teammate.